
The first wave of the COVID-19 pandemic has had a significant effect on the provision of health services in NSW, reducing activity across many areas in ways that could have longer-term consequences on people’s health, new research shows.
The study, published in the Sax Institute’s peer-reviewed journal Public Health Research & Practice, uses administrative data from multiple sources to look at the indirect effects of the pandemic on the NSW health system. It shows how the impact of COVID-19 has reached far beyond actual cases, dramatically altering healthcare-seeking behaviours in the population at the height of the first wave.
The number of breast screens conducted in the period from March to June 2020 dropped by over half compared with the same period in the previous year, the data revealed. Emergency department visits were down by 14%, ambulance incidents by 7% and face-to-face consultations with GPs were down by 22%.
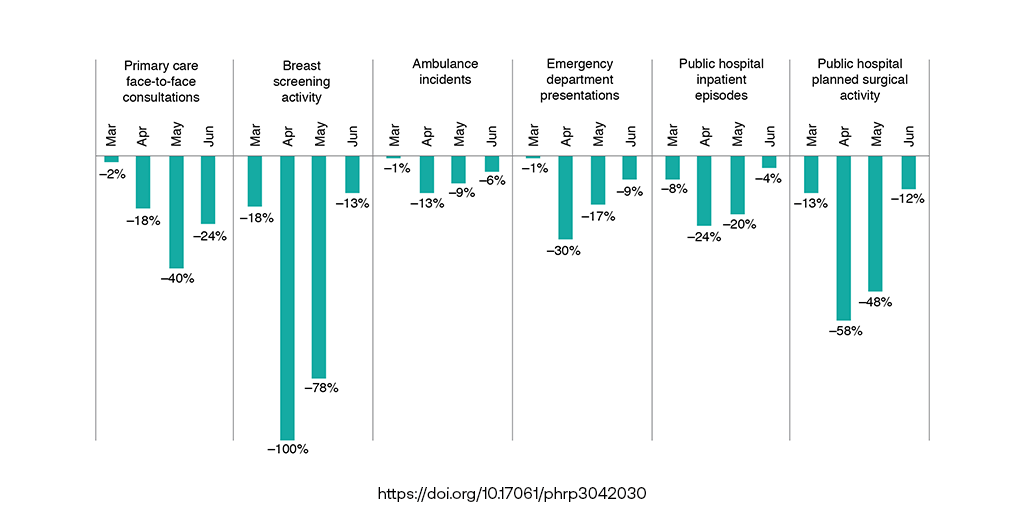
The researchers even found a decrease in people presenting with medical emergencies such as stroke and heart attack.
“Earlier in the pandemic, there were sharp decreases in the number of people presenting to emergency departments. While some of these may be the result of reduction in high-risk activities, some could be related to delays in seeking diagnosis or treatment for life-threatening conditions and could have serious consequences,” said senior author Dr Jean-Frédéric Levesque, Chief Executive of the NSW Agency for Clinical Innovation.
The study also tracked mental health presentations, which declined in April and May when lockdown restrictions were at their most severe, but then ticked up to above the rates of the previous year by June 2020. This uptick may reflect the deleterious effects of the pandemic, and associated restrictions, on mental health, the researchers said, including impacts on people already living with mental health conditions.
However, not all the indirect effects of the pandemic were detrimental: there were lower than usual rates of infectious respiratory diseases other than COVID-19 and also a sharp decrease in trauma-related injuries in March and April, due to the reduction in social and work activities during the lockdown period and increased focus on personal hygiene during the pandemic.
While healthcare activities had begun to recover by July, they still hadn’t returned to usual levels uniformly, the authors noted. Changes seen in NSW were likely to be replicated elsewhere across Australia and globally, depending on the prevalence of the virus and stage of the pandemic, they said, and all healthcare systems need to prepare for the indirect impacts of the COVID-19 pandemic.
The study is part of a special themed issue of Public Health Research & Practice on extreme events and how public health systems can learn and adapt. A perspective article for this issue looks at how extreme weather events, natural disasters and COVID-19 all have the potential to increase the risk of mosquito-borne disease. The author, Dr Cameron Webb of the Marie Bashir Institute for Infectious Diseases and Biosecurity at the University of University of Sydney, says we need to be adaptive in our mosquito control and management strategies across Australia and be aware when enhanced surveillance is needed due to early or late season public health risks associated with mosquitoes.
Another paper in this issue looks at a climate-related mass bat death event in Queensland, which raised the local risk of human infection with bat lyssavirus. The event points to the need for public health units to be prepared for unexpected events of climate change, the authors say.
Two other COVID-related papers in this issue find:
- People with low health literacy – many of whom also suffer chronic disease – have a much poorer understanding of COVID symptoms and ways to prevent infection
- Disruption of Australia’s cancer screening services due to COVID-19 could have major health repercussions, underlining the need for these services to adapt to ensure the population remains covered.
In an editorial for this issue, Guest Editors Dr Jean-Frédéric Levesque and Professor Mark Harris, Executive Director of the Centre for Primary Health Care and Equity at UNSW Sydney, write that extreme events “probe the gaps” in public health systems, stress-testing them for strengths and deficiencies.
“We need a more adaptive system that can learn from these events, adapt in real time and change to address future extreme events. Decision making needs to be sufficiently centralised or coordinated to prevent further fragmentation of responses but decentralised enough to allow adaptation to local context and needs.”
Click here to view the full contents of the latest issue of Public Health Research & Practice.
Media enquiries
Hugo Wilcken, Media Manager, Sax Institute
M: 0451 122 146 E: hugo.wilcken@saxinstitute.org.au
Nyssa Skilton, PHRP Editor
M: 0408 331 262 E: nyssa.skilton@saxinstitute.org.au
Public Health Research & Practice is an open-access, peer-reviewed, Medline-listed quarterly online journal published by the Sax Institute. Click here to subscribe for free.
Please acknowledge Public Health Research & Practice as the source for any stories on our papers.




